Flow paths, CO₂ absorption, and the elegant dance of fresh gas flow
💭 “Some breaths vanish into the air… others find their way back home.”
In the silent theatre of anesthesia, before propofol softens reality and before the monitors begin their rhythmic hum, a quiet choreography unfolds.
A breath leaves the patient, journeys through a maze of valves and chambers, touches the alchemy of soda lime, and returns — refined, cleansed, renewed.
This is the Circle System.Not merely tubing. Not just valves.But a loop of life, where every molecule is guided with intention, precision, and grace.
Welcome to the world where engineering meets biology, physics becomes poetry, and each breath tells a story.
🌬️ The Beginning of the Loop — Why the Circle System Matters
Before diving into the mechanics, pause and imagine:
A young resident stands beside the anesthesia machine for the first time.The APL valve hisses softly. The reservoir bag rises and falls like a mechanical heartbeat.
Their mentor whispers:
“Everything you need to know about anesthesia… is hidden inside this loop.”
Indeed, the circle system is not just equipment. It is the guardian of low-flow anesthesia, the economist of anesthetic gases, and the environmental shield against unnecessary greenhouse emissions.
Why it matters clinically:
- Conserves heat & humidity
- Enables low-flow anesthesia
- Reduces volatile agent consumption
- Minimizes greenhouse gas release
- Provides stable anesthetic depth
- Delivers smooth rebreathing without hypercarbia
In an era pushing for sustainability, efficiency, and precision, the circle system stands at the center — the quiet hero of the OR.
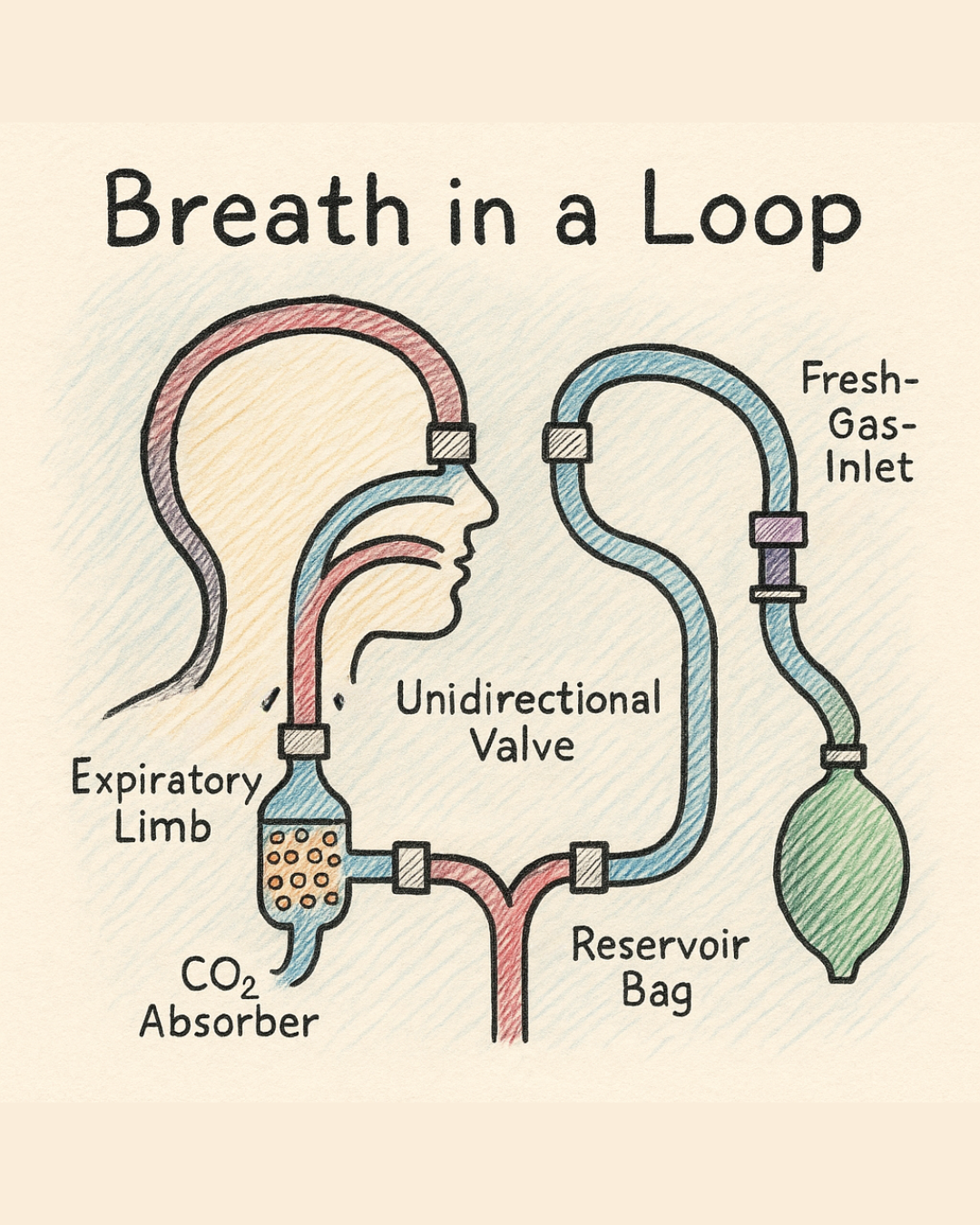
🔧 The Architecture of the Circle — A Loop With Purpose
Think of the circle system as a well-scripted orchestra, where every component has a role, timing, and assigned direction.
Here is the cast:
| 🧱 Component | 📍 Location | ⚙️ Function | 💡 Metaphor |
|---|---|---|---|
| Inspiratory Limb | Absorber → patient | Delivers fresh gas | A road leading inward |
| Expiratory Limb | Patient → absorber | Carries exhaled gas | Journey back home |
| Unidirectional Valves | Inspiratory & expiratory limbs | Maintain one-way flow | Railway gates controlling direction |
| Carbon dioxide (CO₂) Absorber | Between valves | Removes carbon dioxide chemically | A monk that purifies sinful breaths |
| Reservoir Bag | On inspiratory limb | Stores gas and enables manual ventilation | A lung you can hold |
| Adjustable Pressure-Limiting (APL) Valve | Near bag | Controls gas exit and circuit pressure | The system’s escape hatch |
| Fresh Gas Inlet | Near absorber | Adds oxygen and vapor | A tap that replenishes life |
Each part complements the next. Remove or misalign one, and the entire dance collapses.
➡️ The Flow Paths — The Choreography of Gases
Breathing inside a circle system is more like a dance than a simple mechanical exchange. Let’s follow a single breath through its journey.
🟦 The Inspiratory Path — The Clean Return
After purification, gas travels through:
- Inspiratory unidirectional valve
- Inspiratory limb
- Y-piece
- Patient’s lungs
It carries:
- Oxygen
- Anesthetic vapor
- Nitrogen traces
- Water vapor
This is the breath of healing. The breath that sustains anesthesia.
“Inspiration inside a circle system is like the return of a pilgrim — cleansed, purposeful, ready.”
🟥 The Expiratory Path — The Journey of a Used Breath
The patient exhales a mixture of:
- CO₂
- Nitrogen
- Water vapor
- Partially saturated volatile agent
This breath travels through:
- Y-piece
- Expiratory limb
- Expiratory valve
- CO₂ absorber
- Back to mixing chamber
Imagine the breath as a traveler carrying stories —the absorber listens, removes the carbon dioxide, and sends it back purified.
🧪 CO₂ Absorption — The Alchemy of Soda Lime
If engineering built the circle system, chemistry keeps it alive.
Inside the CO₂ absorber lies soda lime — a mixture of:
- Calcium hydroxide
- Water
- Sodium hydroxide (sometimes)
- Potassium hydroxide (older versions)
- Silica binders
When CO₂ from exhaled gas enters the canister, a chemical ballet begins.
The Reaction (simplified):
CO₂ + H₂O → H₂CO₃
H₂CO₃ + Ca(OH)₂ → CaCO₃ + 2H₂O + heat
Why the canister becomes warm
These reactions are exothermic — they release heat.The warmth you feel is the absorber whispering:
“Yes, I’m doing my job.”
Signs the absorber is failing:
- Rising EtCO₂
- Color change (white → purple)
- Cooling of canister
- Hard granules (desiccation)
- Sudden rise in inspired CO₂
Channeling — The Silent Enemy
If gas follows predictable small paths (channels), CO₂ escapes absorption.Like water bypassing a filter.
🧩 Clinical Pearl
A warm canister is comforting; a cold one during a case should make your heart race.
🌬️ The Elegant Dance of Fresh Gas Flow
Fresh Gas Flow (FGF) is the circle’s conductor. It decides how much rebreathing occurs, how quickly anesthetic concentration changes, and how efficiently the system runs.
Let’s break it down.
🌪 High-Flow Anesthesia (≥4–6 L/min)
- Minimal rebreathing
- Fast induction/wash-in
- Similar to open system
- High agent consumption
“High flow is loud generosity — everything is given, nothing saved.”
🌤 Medium-Flow (1–2 L/min)
- Partial rebreathing
- Common in modern practice
- Efficient, controlled, safe
- Good humidity preservation
🌱 Low-Flow (0.5–1 L/min)
- High rebreathing
- Excellent cost savings
- Requires vigilance
- Enhances humidity and temperature
“Low flow is quiet wisdom — saving, sustaining, harmonizing.”
🌎 Minimal or Closed-Loop Flow (<0.5 L/min)
- Advanced technique
- Near-complete rebreathing
- Demands precise monitoring
- Eco-friendly & highly efficient
🔄 Rebreathing Dynamics — The Science Behind the Loop
Rebreathing, when guided well, is not a flaw. It is a feature — the hallmark of efficiency.
What is rebreathing?
Reinhalation of exhaled gases after CO₂ removal.
What gets rebreathed?
- Oxygen
- Anesthetic vapors
- Nitrogen
- Water vapor
What does not return?
- Carbon dioxide (removed)
Rebreathing reduces:
- Agent wastage
- Heat loss
- Humidity loss
- Oxygen wastage
It stabilizes:
- Anesthetic depth
- Gas composition
- Physiological comfort
📚 Mini-Story — “The Breath That Found Wisdom”
A breath left the patient carrying fatigue (CO₂). It wandered through the system like a traveler in need of cleansing.At the absorber, its burdens were lifted.
It re-entered the lungs lighter, warmer, wiser.
Rebreathing is not recycling —it is refinement.
⚠️ Pitfalls, Pearls & Life-Saving Clues
Even the finest systems need vigilance.
Common Pitfalls:
❌ Faulty one-way valve → hypercarbia
❌ Exhausted absorber → rising ETCO₂
❌ Circuit leak → loss of volume/pressure
❌ Desiccated soda lime → carbon monoxide generation
❌ High resistance → increased work of breathing (esp. pediatrics)
Clinical Pearl Box
💎 Breathing circuits tell stories — if you listen.
A fluttering valve.
A cooling absorber.
A rising ETCO₂.
Each is a message in code.
♻️ Environmental & Economic Brilliance
Circle systems are foundational to green anesthesia.
Environmental Benefits
- Reduced greenhouse gases
- Lower volatile agent release
- Sustainable OR practice
Economic Benefits
- Reduced anesthetic consumption
- Cost savings during long surgeries
- Improved humidity → reduced respiratory complications
“When the circle breathes wisely, the planet breathes easier.”
🧠 Advanced Insights (Made Simple)
Even complex physics becomes intuitive inside the circle.
Fresh Gas Decoupling
Prevents FGF from altering tidal volume.
Vital for precise ventilation.
Compliance Dynamics
Circuit compliance absorbs some volume before patient receives full VT.
Dead Space Management
Circle system has minimal apparatus dead space due to valve placement.
Laminar vs Turbulent Flow
Impacts resistance; circle systems designed to minimize turbulence.
🔚 Conclusion — The Loop That Never Ends
The circle system is more than a breathing circuit.It is a symbol of continuity, a blend of chemistry, physics, physiology, and art.
Every breath inside it is guided, refined, and returned with purpose.
“A circle has no end — and neither does the anesthesiologist’s vigilance.”
Master the loop, and you master one of anesthesia’s most elegant secrets.
📚 References & Bibliography
- Miller’s Anesthesia, 10th Edition.
- Dorsch & Dorsch. Understanding Anesthesia Equipment, 6th Ed.
- Feldman JM. Low-flow anesthesia. Anesth Analg. DOI: 10.1213/ANE.0b013e31821
- Mapleson WW. Breathing systems analysis. Br J Anaesth.
- Saini V et al. Carbon dioxide absorption technologies. J Clin Monit Comput.
- Baum J. Soda lime dynamics. Anesth Analg. DOI: 10.1097/00000539-2003
Leave a Reply